Can Continuous Glucose Monitor (CGM) Patches Cause Allergies? What You Need to Know
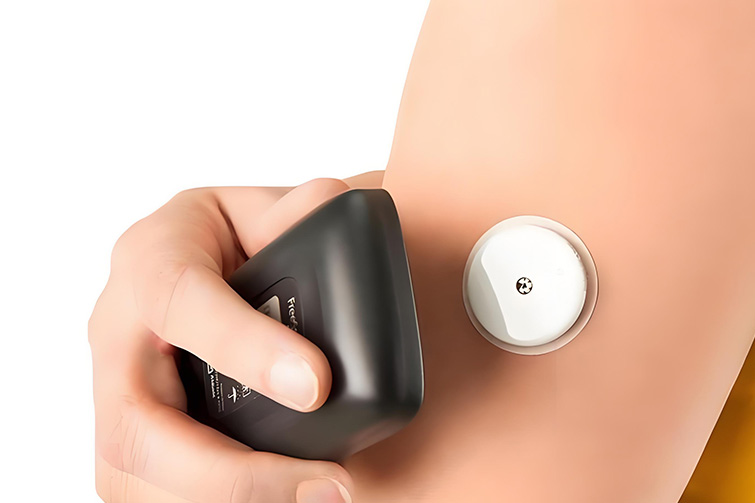
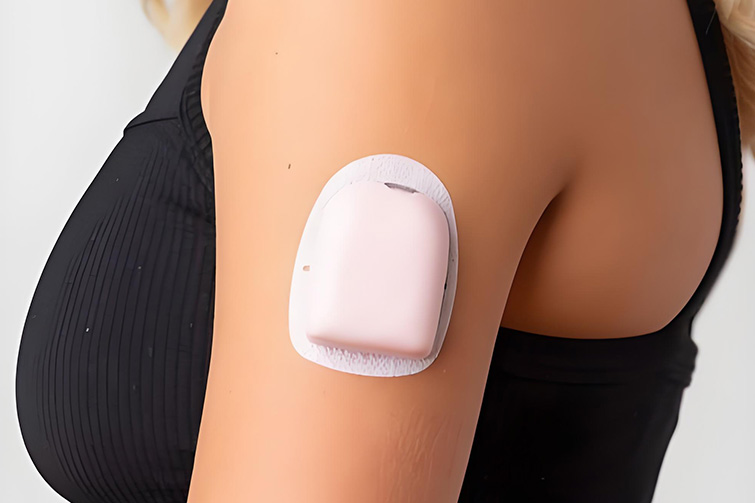
Continuous glucose monitors (CGMs) like Dexcom, FreeStyle Libre, and Medtronic Guardian have transformed diabetes management. These small sensors, worn on the skin for 7 to 14 days, provide real-time glucose readings without fingersticks. But for a growing number of users, a frustrating problem arises: red, itchy, irritated skin under the patch. So, can CGM patches actually cause allergies? The short answer is yes — but the reasons are often more complex than a simple allergic reaction. This article explains what happens, why it occurs, and how to prevent or manage skin reactions.
Allergic reaction vs. skin irritation: two different problems
First, it is important to distinguish between a true allergic reaction (mediated by the immune system) and irritant contact dermatitis (a non-allergic skin irritation). Both can look similar: redness, itching, swelling, and sometimes small blisters or peeling skin. However, their causes and long-term management differ.
- True allergic contact dermatitis occurs when your immune system recognizes a specific chemical in the CGM patch as a foreign threat. This typically appears 24–72 hours after applying a new sensor, and the rash often spreads beyond the edges of the patch. It tends to worsen with each subsequent use.
- Irritant contact dermatitis is much more common. It happens when the skin’s protective barrier is damaged by friction, moisture, adhesives, or trapped sweat. The reaction usually stays within the exact shape of the patch and appears within a few hours to a day. It often improves if you change application techniques or use skin barriers.
What ingredients in CGM patches cause allergies?
CGM patches consist of several layers: a medical-grade adhesive, a backing material (often polyester or polyurethane), and sometimes a protective film. The adhesive itself contains multiple chemicals, and any of them can trigger a true allergy in susceptible individuals. The most common culprits include:
- Acrylates – These are the main sticky components in many medical adhesives. Acrylate allergy is well-documented and can be severe. It is also found in surgical tapes, artificial nails, and some glues.
- Colophony (rosin) – A natural resin derived from pine trees, used as a tackifier in adhesives. It is a frequent allergen.
- Methacrylate monomers – Some CGM patches use UV-cured acrylic adhesives that may contain residual monomers, which are potent allergens.
- Urethanes and polyurethanes – Less common, but possible triggers.
- Preservatives – Such as parabens or benzisothiazolinone, added to prevent bacterial growth in the adhesive.
If you suspect a true allergy, a dermatologist can perform patch testing with a standard series (including acrylates and colophony) to identify the exact trigger.
Why are CGM reactions becoming more common?
Several factors explain the rising reports of skin reactions to CGM patches:
- Longer wear time – Modern CGMs last 7, 10, or even 14 days. Prolonged adhesive contact increases cumulative irritation and the chance of developing sensitization over time.
- Water exposure – Showering, swimming, and sweating break down adhesives and trap moisture against the skin, leading to maceration (soft, white, wrinkled skin) and irritation.
- Repeated application – Users apply a new sensor every 1–2 weeks, year after year. Repeated exposure to the same chemicals can convert a mild irritation into a true allergy (sensitization).
- Tighter adhesives – To keep sensors from falling off, manufacturers use stronger glues. Stronger glues contain more aggressive chemicals.
Symptoms to watch for
Mild to moderate reactions include:
- Redness confined to the adhesive area
- Itching (mild to intense)
- Dry, scaly, or cracked skin after patch removal
- Small bumps (papules) or vesicles (tiny blisters)
Severe reactions (less common) include:
- Blistering with clear or yellow fluid (weeping)
- Intense burning pain
- Spreading rash beyond the patch site
- Open sores or crusting
If you develop severe symptoms, remove the sensor immediately and consult a healthcare provider. Do not reapply another sensor to the same spot until the skin has fully healed.
How to prevent and manage CGM patch allergies
Before giving up on CGM technology, try these proven strategies.
1. Use a skin barrier preparation
Apply a liquid skin barrier (e.g., Skin-Tac, Cavilon No-Sting Barrier Wipe) or a hydrocolloid dressing (cut a hole for the sensor filament) between your skin and the adhesive. These products create a physical layer that reduces direct contact with allergenic chemicals. Many users with mild allergies tolerate CGMs perfectly with a barrier.
2. Try an underpatch
Specialized CGM underpatches (made of thin, breathable fabric with a hypoallergenic adhesive) are placed on the skin first; then the sensor goes on top. Brands include Not Just a Patch, GrifGrips, and Simpatch. Some underpatches are infused with aloe or hydrocolloid material to soothe skin.
3. Change sensor sites more frequently
Even if a sensor claims 14-day wear, consider changing it at 7–10 days if your skin reacts. Rotate sites thoroughly — upper arm, abdomen, upper buttocks (for some CGMs), and thighs (off-label but often possible). Never reuse a site that is still red or tender.
4. Optimize skin preparation
- Clean the site with mild soap and water (not alcohol, which can strip oils and worsen irritation).
- Dry completely before applying the sensor.
- Shave hairy areas (hair traps moisture and bacteria).
- Apply a thin layer of prescription topical steroid (e.g., triamcinolone 0.1%) under the barrier wipe for known allergic users — but only under medical guidance.
5. Consider alternative adhesive formulations
Some CGM brands use different adhesives. For example, Dexcom G7 has a smaller patch and reportedly a modified adhesive compared to G6. Libre 3 uses a different backing material. If you react to one brand, you may tolerate another. Also, third-party hypoallergenic overpatches (like Tegaderm HP or Hypafix) can replace the stock adhesive patch.
When to see a doctor
Consult a dermatologist or your endocrinologist if:
- Home measures fail after 2–3 attempts.
- You develop blisters, open skin, or infection (yellow crust, spreading redness, warmth).
- The reaction affects sleep or daily function.
- You want patch testing to identify the exact allergen.
In some cases, doctors prescribe topical steroids to apply before sensor placement, or systemic antihistamines for severe itching. Very rarely, a patient may need to switch back to fingerstick monitoring or use a different CGM technology.
The bottom line
Yes, CGM patches can cause allergic reactions, but true acrylate allergy is uncommon. The vast majority of skin problems under CGMs are irritant contact dermatitis caused by moisture, friction, or prolonged wear. Fortunately, most reactions can be prevented or managed with skin barriers, underpatches, proper site rotation, and good skin preparation. Do not suffer in silence — and do not abandon your CGM without trying these solutions. Modern diabetes technology is too valuable to give up over a fixable skin issue. If you continue to struggle, an allergist or dermatologist can help you find a safe, long-term way to wear your CGM comfortably.





